Summer 2023
Where do Your Members Receive Care?
Fair Health has just released its 2023 Healthcare Indicators and Medical Price Index White Paper, and the data shows where members receive care can have a big impact on their employer’s health spend. Pricing for the same ‘new patient outpatient visit’ can vary drastically depending on where care is received and how long the visit takes.
Price Comparison: Office, Urgent Care Center & Retail Clinic (2021)
Percentage of Employees Enrolled in HDHP (2021)
| CPT Code | Office | Urgent Care | Retail Clinic |
|---|---|---|---|
| New patient outpatient visit, total time 15-29 minutes (CPT code 99202) | $141 | $200 | $99 |
| New patient outpatient visit, total time 30-44 minutes (CPT code 99203) | $226 | $240 | $139 |
| New patient outpatient visit, total time 45-59 minutes (CPT code 99204) | $350 | $329 | $348 |
| New patient outpatient visit, total time 60-74 minutes (CPT code 99205) | $450 | $410 | NA* |
With a self-funded plan from TPSC, your employees have convenient access to care when they need it. We’ve partnered with many local and national PPO networks to bring affordable care to members no matter their location.
IRS Announces 2024 HSA and EBHRA Contribution Limits, HDHP Minimum Deductible, and HDHP Out-of-Pocket Maximums
| HSA | 2023 | 2024 |
|---|---|---|
| Self-Only Contribution Limit | $3,850 | $3,850 |
| Family Contribution Limit | $7,750 | $8,300 |
| HDHP (Self-Only Coverage) | 2023 | 2024 |
|---|---|---|
| Minimum Deductible | $1,500 | $1,600 |
| Maximum Out-of-Pocket Limit | $7,050 | $8,050 |
| HDHP (Family Coverage) | 2023 | 2024 |
|---|---|---|
| Minimum Deductible | $3,000 | $3,200 |
| Maximum Out-of-Pocket Limit | $15,000 | $16,100 |
| EBHRA | 2023 | 2024 |
|---|---|---|
| Limit | $3,000 | $3,200 |
High-Cost Claims on the Rise
A recent report from Sun Life shows claims over a million dollars increased 45% from 2019-2022. In 2019, 109 claims per million covered members were over one million dollars, and in 2022, 158 claims per million covered members were over that threshold.
Like specialty medication, high-cost claims are a major cost-driver for self-funded plans. Without the right stop-loss carrier, many organizations cannot sustain the continued treatment many of these claims require. That’s why we’ve partnered with industry-leading partners to bring affordable stop-loss coverage to our clients, ensuring you can provide the care your employees need.
The Value of Employer-Provided Coverage in 2023
A nationwide survey of 1,000 consumers reflected that over 60% are satisfied with their employer-sponsored healthcare benefits, and quality healthcare coverage is one of the driving factors of employee retention.
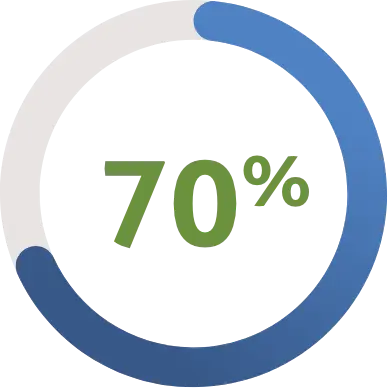
Nearly 70% prefer to get their coverage through their employer instead of the government.
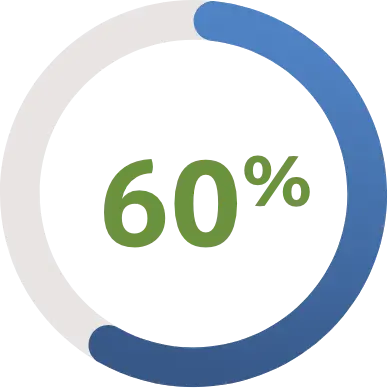
Feel the quality of their health insurance plan is high.
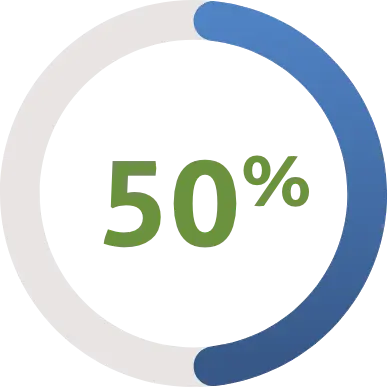
Over 50% feel what they pay for coverage is reasonable.
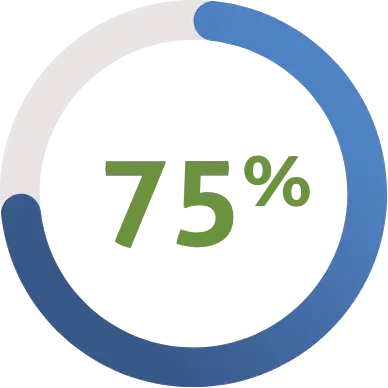
Almost 75% of respondents believe it’s important to maintain the COVID-19 telehealth flexibilities.
At TPSC, we customize plans to fit the exact needs of any organization, no matter the size. With proven cost-containment solutions, extensive PPO networks and top-of-the-line customer support, our clients are seeing real savings from switching to self-funding.
ACA Preventive Health Services Mandate to Remain in Effect During Braidwood Appeal
Background:
In Braidwood v. Becerra, a group of employers and individuals have challenged the ACA’s Preventive Health Services Mandate, specifically as it relates to the coverage requirements triggered by recommendations from the United States Preventive Services Task Force (USPSTF). The group argues that the mandate is unconstitutional as a whole, and the 2019 USPSTF recommendation requiring employers to cover HIV preexposure prophylaxis (PrEP) violates the Religious Freedom Restoration Act (RFRA).
The trial court held that requiring coverage of PrEP does violate the RFRA, and that the USPSTF lacked the authority to determine preventive services that must be covered by private health plans. They also vacated all HHS, IRS and DOL actions taken on or after March 23, 2010, to implement or enforce the preventive health services mandate in response to USPSTF recommendations.
The Latest:
The government appealed the court’s decision, and asked the appellate court to put on hold the trial court’s ruling during the appeal. Now, the appellate court is allowing the USPSTF’s recommendations to remain in effect while the case is decided. The government also agreed to not take enforcement action against the employers who brought the lawsuit (or their insurers) for their refusal to cover otherwise-required preventive services during the hold period.
If you have any questions on how this ruling impacts your specific plan, please contact your dedicated TPSC Account Manager.

